 Source of graph: online version of the WSJ article cited below.
Source of graph: online version of the WSJ article cited below.
(p. A1) Four years ago, Paluxy Valley Physicians of Glen Rose, Texas, was struggling to recoup more than $500,000 in denied or unpaid claims from insurers. Two of its eight doctors left the practice, while three others had to borrow $100,000 to keep it afloat.
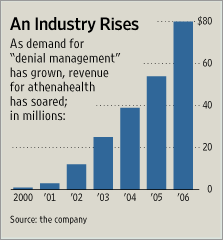
To turn things around, the medical practice turned to Boston-based athenahealth Inc., one of the biggest of hundreds of companies in a lucrative niche: helping doctors wring payments from health plans. Athenahealth’s software flagged and corrected the complex coding for thousands of claims, preventing them from getting hung up in insurers’ Byzantine rules. Today, Paluxy Valley has whittled its claims outstanding to $179,000 and repaid the bank loan. No longer in a revenue crunch, its doctors have stopped moonlighting in the emergency room to make money.
"The insurers outcode us, they outsmart us and they have more manpower," says Shari Reynolds, the administrator at Paluxy Valley, which pays athenahealth a little over 3% of the $2.5 million it collects annually from insurers. "Now at least we have a fighting chance."
Doctors increasingly complain that the insurance industry uses complex, opaque claims systems to confound their efforts to get paid fairly for their work. Insurers say their systems are designed to counter unnecessary charges and help keep down soaring health-care costs. Like many tug-of-wars over the health-care money pot, the tension has spawned a booming industry of intermediaries.
It’s called "denial management." Doctors, clinics and hospitals are investing in software systems costing them each hundreds of thousands of dollars to help them navigate insurers’ systems and head off denials. They’re also hiring legions of firms that dig through past claims in search of shortchanged payments and tussle with insurers over rejected charges. "Turn denials into dollars," promises one consultant’s online advertisement.
The imbroglio is costing medical providers and insurers around $20 billion — about $10 billion for each side — in unnecessary administrative expenses, according to a 2004 report by the Center for Information Technology Leader-(p. A18)ship, a nonprofit health-technology research group based in Boston.
For the full story, see:
(Note: I noticed some minor differences between the titles and texts of the print and online versions. My excerpt gives the online version.)
